
Research Summary
Cost savings for pediatric care can be achieved by investment in...
(1) promoting comprehension of medical vocabulary in the preferred language (where the language barrier is not the reason for health literacy disparities), and ways to care for young children and their parents and supporting awareness of the available social support services and patient navigation for access to preventative primary care or specialty health care services rather than emergency room visits when possible.
(2) public health systems and educational settings are ideal support venues, (now advocating for intermittent preschool opennings and available spaces to offset housing crowding and technology access with stay at home requirements due to pandemic) for family support, and supports for reducing risk factors impeding learning for educational endeavors).
(3) Parent education and referrals work to get families to primary care even when some families who typically prefer not to go to primary care, they actually like primary care once they attend! Therefore, both options, possibly more preschool visits or home visiting would work in lieu of only going to pediatric care.
The Background Story...
In 2007 to 2012 Delaware reported that they ranked last or up to 26th in the nation for achieving the completion of developmental screenings to determine achievement of a child's milestones or identification of need for early intervention for those with developmental disability or delay. When the task was designated to preschools instead of pediatric primary care, another disparity arose with access to either. Lower ability to obtain, process, and access health information results in costly emergency room overusage, and poor health management and health outcomes, especially for twenty percent of children below age 5 living in poverty and coping with obesity and related conditions results the risk factors for worse pediatric health outcomes. Past health literacy studied adolescent and adult health literacy in clinical settings in English only. This study reviewed Nonclinical settings for parental health literacy, parent education, screenings and referrals.
Voluntary participation in survey research was completed with 220 parents from 12 Head Start and Non Head Start preschools in New Castle County, Delaware. Four paper surveys,administered in English and Spanish, Green and Kreuter's 2005 Precede-Proceed model is applied to an original logical model for determining a need for a preschool health literacy intervention to inform better child health outcomes. Results indicate that low-income, minority families, have fewer health books at home, which is associated with lower parental health literacy, higher child BMI, and more health care referrals for managing childhood obesity. Lower Nutritional/ Functional health literacy scores for understanding health information disproportionately affected minority families in Head Start programs for Hispanic families, and Black families respectively, even when surveys were administered in Spanish, or the preferred language. Head Start preschools offer more parent health education and twice the rate of referrals to primary care as Non Head Start programs for the families to attain the same level of health seeking behavior.
Low Parental Health Literacy Causes Unnecessary Healthcare Expenditures from Emergency Room Overuse!
Completion of Developmental Screenings are the intervention because referrals get families to primary care or early intervention once the preschools and parents work together to complete this task identifying the celebration of children's reaching their milestones, experiencing natural delays or needing support through early intervention.
It is more economical to have regular primary care visits than go to rely on the more expensive emergency room for care (Herman & Jackson, 2010; Sanders, Shaw, Guez, Baur, and Rudd, 2009). In 2007, approximately 18 billion dollars was estimated to be spent in avoidable emergency room use in the United States (Cook, Hicks, O’Malley, Keegan, Guadagnoli, & Landon, 2007). Many low-income families, continue to address health concerns at the emergency room instead of having a routine primary care physician, (Herman & Jackson, 2010). Therefore, early education and care (EEC) programs are an ideal potential intervention site for preventable health care conditions including chronic health problems like obesity. Representing 7 to 17 percent of personal health expenditures, some reports estimate that the cost of low health literacy to the U.S. economy is between $106 billion to $238 billion annually (Vernon, Trujillo, Rosenbaum, DeBuono, 2018). Therefore, in order to offset unnecessary expenses, identifying earlier needs and points of intervention are necessary.
This study explores disparities in parental health literacy and preschool provided healthcare referrals for preschool age children who may have weight management problems. The inquiry will clarify needs for promoting parental health literacy and early intervention needs for child weight management in relation to health seeking behavior for pediatric primary care. More specifically, because there are larger numbers of disadvantaged children in Head Start programs vs non Head Start programs, it is important to consider what differences in school type may mean for addressing the needs of enrolled parents and children. Programs like Head Start that serve economically disadvantaged children may compensate for low-income risk factors for childhood obesity by offering more parent education programs and referrals in contrast with Non-Head Start programs. This compensating effort may help to get families to pediatric primary care and medical homes, who otherwise would not know when, where, and how to seek health care for young children with chronic illness issues, due to low parental health literacy. It is also important to recognize that parent education alone may not be sufficient for implementing a behavior change towards a status of good or optimum health. It is important to understand disparities in parental health literacy skills because this effort informs a knowledge asset or risk base for child health status. Furthermore, preschool provided health education and referrals to get the family to health support at pediatric primary care may vary according to parental health needs and cultural notions about health seeking behavior.
Research Focus
The focus of the research is on how parents from different income groups differ in functional and nutritional health literacy scores, and to what extent early education and care (EEC) programs, which provide care for income specific groups, differ in resulting children’s health outcomes measured by child BMI. The results then reflect a varying need for health care referrals and pediatric health care utilization. For example, federal funding responds robustly through program standards to supporting (low) income eligible families to receive comprehensive EEC services in order to bridge the gap in quality of services allotted by private pay or state subsidies for higher income groups. It is important to check for the level of parent education support provided to these non-federally funded families, whose children also exhibit weight management problems. Although parents from higher income groups may have higher educational attainment, many people still struggle with navigating the health care system. Without adequate parental health literacy and parent health education, in either income group, it is possible that less optimum attainment for children’s health in weight management still occurs due to lack of health literacy skills or EEC programmatic differences.
Preschool standards and policies like Stars QRIS standards support better quality care regardless of funding streams. Based on examination of the literature, the main outcome variable is health seeking behavior as a function of characteristics associated with parental health literacy. The following variables may be associated with health literacy scores: demographic factors (age, race/ethnicity, and education attainment level), number of health books at home, and parent health education. The consequent child BMI status and frequency of health care referrals result in a level of health seeking behavior in combination with perceptions of health care quality.
The quantitative research design studies parents of young children attending twelve high quality preschools in New Castle County, Delaware. Because the schools were selected for being high quality, it is known that they were all required to complete developmental screenings, which otherwise might impact the rate of health care referrals. Data from four parent surveys request information from voluntary responses about: 1) demographics including home health literacy environment, 2) parent functional and nutritional health literacy score, 3) preschool provided nutrition and physical activity education, and 4) perceptions of health care quality and health seeking behavior.
Example Curriculum

Basic Statistics Concepts p1
Use this block to showcase testimonials, features, categories, or more. Each column has its own individual text field. You can also leave the text blank to have it display nothing and just showcase an image.

Basic Statistics Concepts p2
Use this block to showcase testimonials, features, categories, or more. Each column has its own individual text field. You can also leave the text blank to have it display nothing and just showcase an image.

Basic Statistics Concepts p3
Use this block to showcase testimonials, features, categories, or more. Each column has its own individual text field. You can also leave the text blank to have it display nothing and just showcase an image.

Research Questions

Research Questions continued

Data Analysis
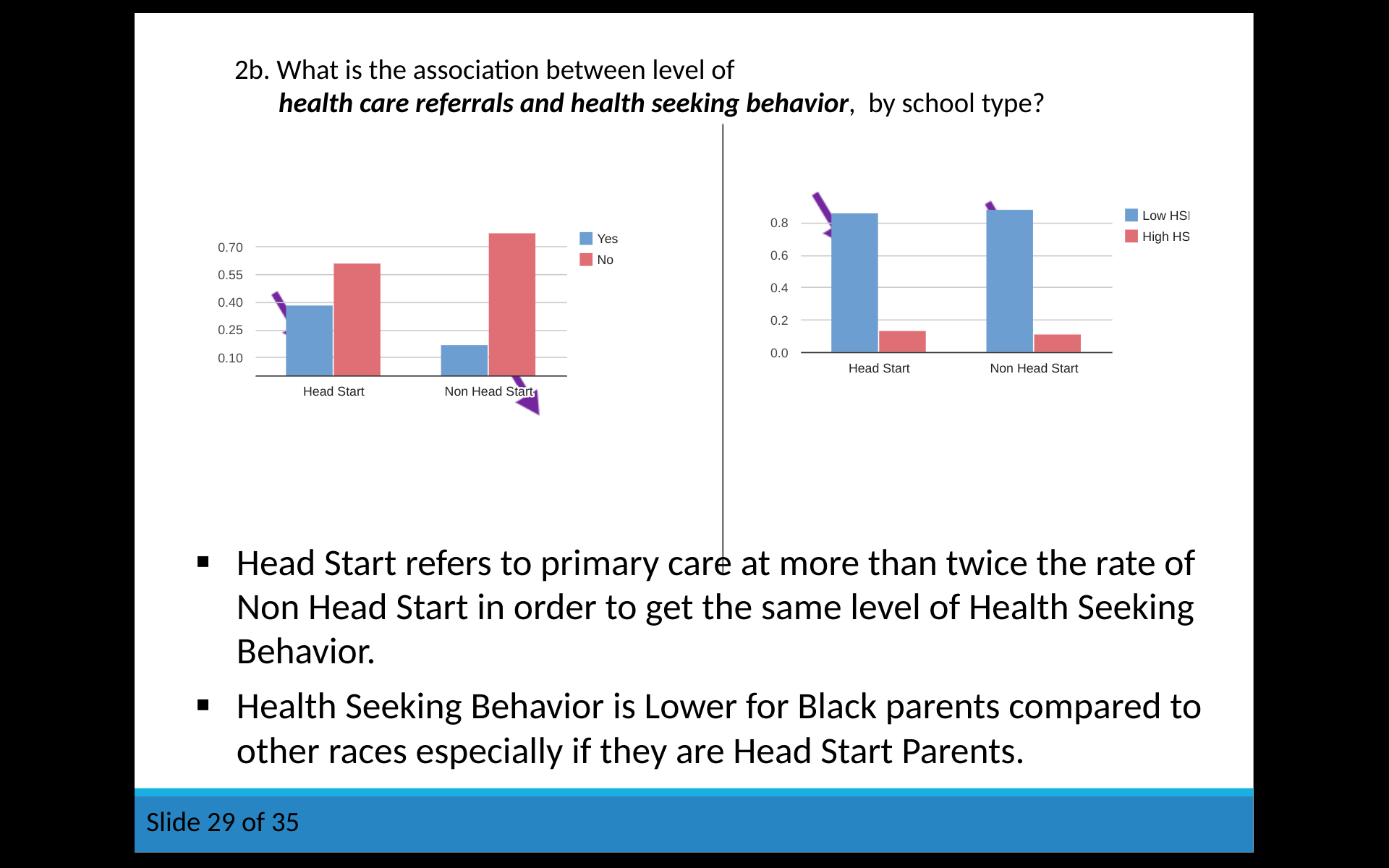
Bar Graph

Example of a Survey, what is the mistake?
Answer, need to include two categories, (1) 18 years of age and older, and (2) Less than 18 years of age so that age ranges don't overlap and are considered exclusive from one another.
This is called "mutually exclusive" answer choices.

Example of a APA writing for
Chi Square results, for levels of association between categorical variables
Use this block to showcase testimonials, features, categories, or more. Each column has its own individual text field. You can also leave the text blank to have it display nothing and just showcase an image.

